What is Capsular Contracture?
)
1. What is Capsular Contracture?
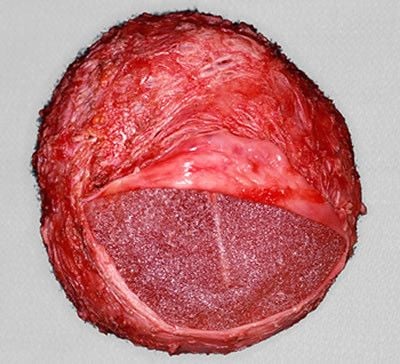
Capsular Contracture is a tightening of the scar tissue that forms around the breast implant. The scar tissue is normal and is known as the 'capsule', and the tightening is referred as 'contracture'. This is also often known as 'hardening' of the breast due to breast implant surgery. Mild contractures can feel firm. More severe contractures can be painful and may distort the breast by pulling the breast implant up significantly.
2. Why does it happen?
There are several theories, all of which plays an integral part in the formation of capsular contracture.
Your body is smart - your immune system knows when a foreign object has been put into your tissues. In order to isolate the implant, your body creates a sac, or capsule of scar tissue around it, to seal it off. A capsule around a breast implant is a naturally occurring tissue that can be of benefit. If that capsule contracts or thickens, however, it can squeeze and misshapen your implant. This contracture is what will cause pain, shifting, distortion, and hardening of the breast. Some individuals are more prone to developing capsular contracture than others. There is some evidence that if you have had capsular contracture with breast implants, this may recur with replacement as this is the way your body deals with foreign objects.
Capsular contracture can happen around any type of breast implant (both saline and silicone). Sometimes it develops due to postoperative problems such as infection that sneaks in during implant surgery. But other postoperative issues, like a seroma (a pocket of blood serum within the surgical area) or a hematoma (a pool of blood below the skin), may also contribute to the development of capsular contracture.
There have been studies over recently, in the last few years to show that the formation of a biofilm (bacteria and their secretions) on an implant contributes to the formation of capsular contracture.
3. When does capsular contracture occur?
Capsular contracture can occur any time after implant surgery. Sometimes it occurs as soon as 12 months after surgery, other times, it may take years to develop.
4. How can it be prevented?
There has been many studies done on capsular contracture. The factor with the most evidence is submuscular placement of the breast implant (under the muscle), which showed approximately 4% incidence of capsular contracture, compared to 14-20% incidence in subglandular (above the muscle) placement. There has been some evidence to show that textured implants have lower incidence, and that postoperative implant massage can decrease the likelihood of capsular contracture. Radiotherapy is definitely a contributing factor for high risk of capsular contracture in patients who have implant reconstruction.
Due to the theory on biofilms and capsular contracture, and a 14-point plan has been published for implant surgery to minimise implant complication such as capsular contracture.
- Use intravenous antibiotic prophylaxis at the time of anaesthetic induction
- Avoid peri-areolar incisions
- Use nipple shields to prevent spillage of bacteria into the pocket
- Perform careful atraumatic dissection to minimize devascularised tissue
- Perform careful hemostasis
- Avoid dissection into the breast parenchyma.
- A dual-plane pocket has anatomic advantages
- Perform pocket irrigation with correct proven triple antibiotic solution or betadine
- Minimise skin-implant contamination
- Minimise the time of implant opening, reposition and replacement of implant
- Change surgical gloves prior to handling the implant. Use clean or new instruments that were not used in the pocket dissection
- Avoid using a drainage tube, where possible
- Use a layered closure
- Use antibiotic prophylaxis to cover subsequent dental or surgical procedures that produce bacteremia, and have lifelong follow-up
5. How is Capsular Contracture Diagnosed?
The diagnosis of capsular contracture is most commonly based on clinical examination alone. Imaging studies can offer further insight, with MRI being the most accurate test in making the diagnosis. Often, capsular contracture is associated with implant rupture. Capsular contracture can be graded on severity by the Baker Scale:
- Grade I - the breast is soft and appears normal, and the capsule is flexible.
- Grade II - the breast looks normal, but is somewhat hard to the touch.
- Grade III - the breast is hard, has some distortion caused by contracture, or the breast becomes a rounded shape, or the implant is generally tilted upwards
- Grade IV - similar to grade III but with greater hardening of the capsule and is associated with pain.
6. What can I do to avoid capsular contracture?
- Take it easy doing physical activities and avoid injury or impact to the breast. The implant needs time to settle into place, so don't jostle, squeeze, or strike the surgical site at all.
- Massage your breast implants regularly once healed, ask your surgeon for instructions.
- Attend regular breast implant checks with your surgeon (1-2 yearly).
- If you know that you'll be having chest wall radiation after your mastectomy, consider delaying implant surgery until treatments are completed. Radiation following immediate construction is associated with a greater risk of reconstructive failure, and other complications including infections, and capsular contracture, so waiting may be well worth your time.
7. How is capsular contracture treated?
Not all capsular contractures need to be treated. Baker Grade I is normal, while Baker Grade II can often be observed. However, if the breast shape is distorted, if the implant is pushed out of position, or if the hardening causes discomfort, surgery may be recommended. Usually, implant removal with capsulectomy (removal of the hard capsule) is required, and the implant may or may not be replaced during this procedure.
Talk to your surgeon about your options.
To find out more, visit our Breast Implant Revision page.
To read more about breast implants, visit our 'All About Breast Implants' page, or read more blogs on breast implants.
| Tags:plastic surgeryBreast implantsBreast |

